Neurodiversity Celebration Week
Neurodiversity Theme: Inclusion, Ethics, and Psychological Practice in South Africa
Neurodiversity Week 2026 (16–22 March) offers South African psychologists an opportunity not only to raise awareness, but to deepen our ethical commitment to inclusion, dignity, culturally-sensitive, and scientifically grounded practice. As professionals registered with the Health Professions Council of South Africa (HPCSA), our celebration of neurodiversity must extend beyond recognition—it must shape how we assess, diagnose, formulate, and advocate.
Neurodiversity reminds us that differences in attention, communication, learning, sensory processing, executive functioning, and motor coordination reflect natural variation in human brain development. At the same time, diagnostic frameworks such as the Diagnostic and Statistical Manual of Mental Disorders (DSM-5-TR), published by the American Psychiatric
Association (2022), and the World Health Organization International Classification of Diseases (ICD-11) (2019) continue to identify neurodevelopmental conditions that may involve significant functional impairment requiring support. Holding both realities, difference and disability is the ethical task before us.
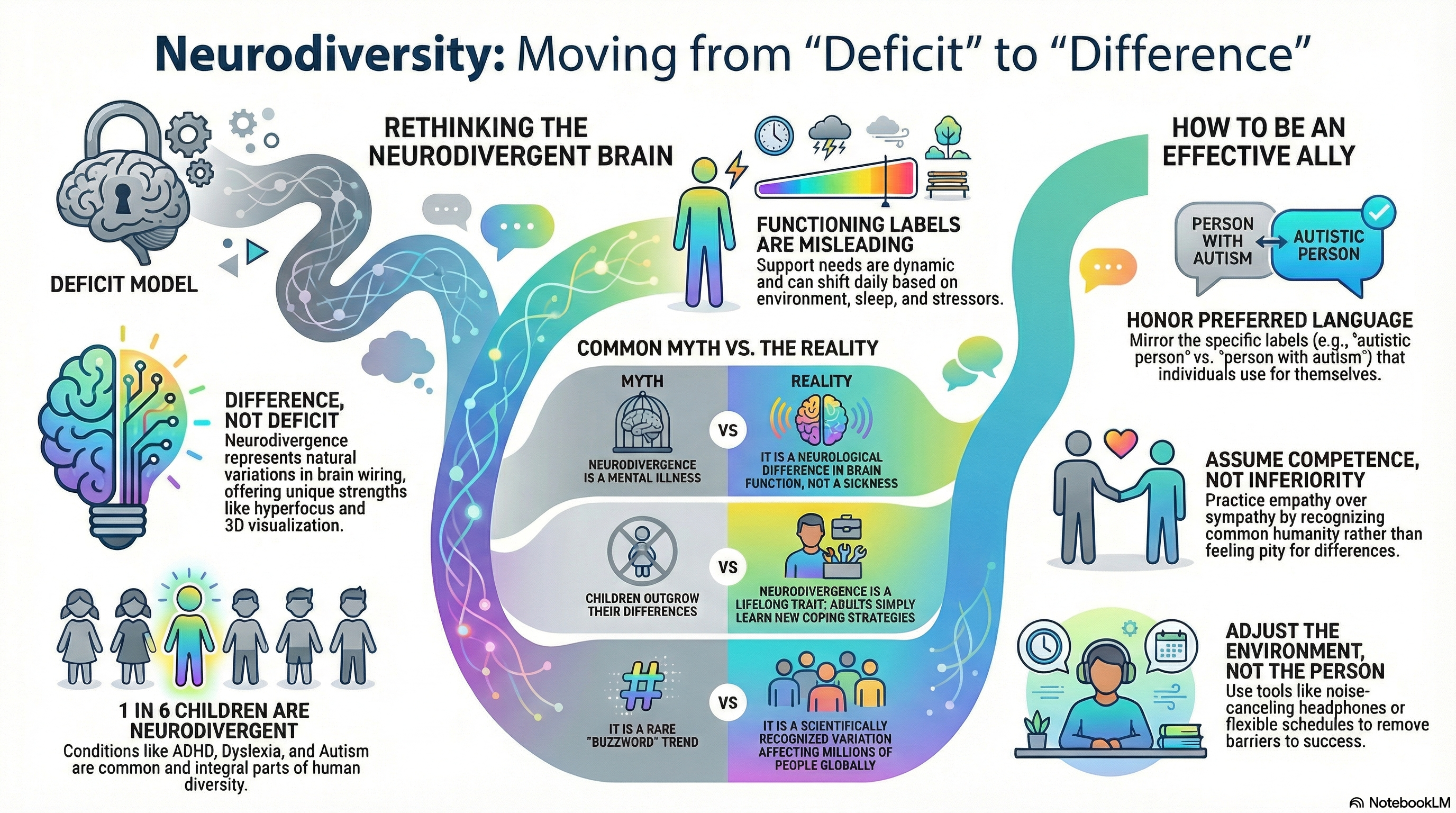
Neurodiversity: Different Wiring, Equal Worth
The concept of neurodiversity, introduced by Judy Singer (1999) and further articulated by Nick Walker (2021), reframes neurological differences as part of natural expected human diversity. Within this paradigm, individuals with autism spectrum disorder, ADHD, specific learning disorders (including dyslexia and dyscalculia), intellectual disability, developmental coordination disorder, tic disorders, and communication disorders are understood as having brain structural and organizational patterns that are “wired differently.”
There is emerging evidence suggesting that even within diagnostic categories, there is significant variation, for example autism is not a single condition with one root cause, but is an umbrella term for a cluster of conditions with similar, although not identical, features. There is likely to be further subgroups identified in future research, leading to more targeted interventions. There are also suggestions that there is a relative under-diagnosis of neurodivergent patterns in communities that lack financial resources, typically those from Black communities.
However, different neurological wiring must not be grounds for exclusion.
- Exclusion arises not from neurological difference itself, but from social environments that are structured around narrow cognitive norms. When schools demand uniform learning styles, when workplaces privilege rigid executive functioning patterns, or when therapeutic spaces assume neurotypical communication styles, systemic barriers emerge.
- As psychologists, our responsibility is to identify not only different patterns of neurological processing and impairment, but also environmental mismatch.
HPCSA Ethics and Inclusion
The HPCSA’s General Ethical Guidelines for the Health Care Professions and Scope of Practice for Psychologists provide a clear framework for Neurodiversity Week reflection. Core principles include:
- Respect for persons and human dignity
- Non-discrimination
- Beneficence and non-maleficence
- Professional competence
These are not abstract ideals. They are practical and professional obligations.
When we use stigmatizing language, overpathologising difference, conflate socioeconomic and language disadvantage with cognitive impairment, or recommend unnecessarily restrictive placements, we risk contravening these principles as set by HPCSA.
Conversely, when we provide balanced diagnostic feedback, advocate for reasonable accommodation in a workplace, and contextualize functional challenges, we actively uphold ethical practice. Celebrating Neurodiversity Week therefore means aligning our Clinical work with our ethical commitments.
Neuropsychologists: Balanced Interpretation Matters
Neuropsychological assessment carries significant consequences for educational access, occupational opportunity, and self-concept.
Contemporary research indicates that conditions such as ADHD and autism involve differences in neural connectivity and developmental timing rather than simple deficits. Reports that emphasize only weaknesses risk reinforcing low expectations. Reports that ignore impairment may limit access to support.
During Neurodiversity Week, Neuropsychologists are reminded that balanced profiling should document strengths alongside challenges, supporting inclusion while maintaining diagnostic rigor.
Workable Sound Commitments for Neurodiversity Week 2026
As we mark 16–22 March 2026, it is essential for psychologists to continuously reflect on the following commitments:
- Update assessment practices to ensure cultural and linguistic appropriateness.
- Review report language for unintended deficit framing.
- Strengthen CPD in neurodevelopmental science.
- Engage in conversations about inclusive policy within schools and organizations.
- Validate neurodivergent identity while addressing functional challenges.
Small shifts in language formulation, recognize differences and practice inclusiveness could have a profound impacts on dignity and belonging.
Beyond Awareness: A Professional Responsibility
Neurodiversity Week is not simply a celebration of difference; it is a reminder of responsibility towards society. Diagnostic clarity remains essential. Functional impairments are real and require structured support. Yet neurological difference does not diminish worth, capacity, or the right to participation in all aspects of broader society
For all psychologists registered with HPCSA; inclusion is embedded within ethical practice. Our role is not to eliminate difference, nor to idealize it, but to ensure that difference does not lead to exclusion but to understanding and inclusion. As we celebrate Neurodiversity Week 2026, may we reaffirm that different brain wiring is part of human diversity and that ethical psychological practice demands understanding, accommodation, and inclusion in society.
The Role of Psychologists during Neurodiversity Week
During Neurodiversity Week and beyond; each category of psychologist registered with the Health Professions Council of South Africa (HPCSA) could play a meaningful role in promoting awareness, inclusion and support.
The brief reflections below highlight possible intersections between neurodiversity awareness and the various categories of psychological practice. These links are offered in a spirit of professional reflection and do not constitute determinations of scope or regulatory guidance, which remain the responsibility of the HPCSA:
- Neuropsychologist: Neuropsychologists Specialized category focusing on neuropsychological assessment, diagnosis and rehabilitation related to brain-functioning disorders. Relevant to neurodiversity where neurological functioning impacts cognition and behavior.
Link: https://www.hpcsa.co.za/board/psychology/regulations.
- Clinical Psychologist: HPCSA Psychology Scope Regulations – Clinical Psychologists Section. Registered to assess, diagnose and treat psychological distress and psychopathology using evidence-based psychological interventions.
https://www.gov.za/sites/default/files/gcis_document/201409/34581rg9582gon704.pdf
- Counselling Psychologist: Link: HPCSA Psychology Scope Regulations of Counselling Psychologists Section. Relevant to neurodiversity when addressing adjustment, identity and related psychosocial issues.
https://www.gov.za/sites/default/files/gcis_document/201409/34581rg9582gon704.pdf
- Educational Psychologist: Assesses and intervenes to optimize learning, development and barriers to learning across the lifespan; includes profiles that relate to neurodiverse conditions. https://www.gov.za/sites/default/files/gcis_document/201409/34581rg9582gon704.pdf
- Research Psychologist: Conducts psychological research often contributing to knowledge on neurodiversity, Link: HPCSA Psychology Scope Regulations Research Psychologists Section
https://www.gov.za/sites/default/files/gcis_document/201409/34581rg9582gon704.pdf
- Industrial Psychologist: less directly neurodiversity-focused, but may assess and advise on workplace adjustment and functioning HPCSA Psychology Scope Regulations – Industrial Psychologists Section
https://www.gov.za/sites/default/files/gcis_document/201409/34581rg9582gon704.pdf
- Registered Counsellor (Psychological), identify needs requiring advanced assessment (e.g., neurodevelopmental concerns), and refer appropriately. Link: HPCSA Psychology Scope Regulations – Registered Counsellors Section
https://www.gov.za/sites/default/files/gcis_document/201409/34581rg9582gon704.pdf